Unless the service is delivered in an emergency setting, all hospital-based services – both inpatient and outpatient – require prior authorization. All outpatient hospital-based requests of service, and even elective inpatient admissions, require hospital prior authorization.
In the present day, finding resources is becoming a huge challenge for many hospitals and health systems. Document filing, following up with the payers, and creating a process that quickens the process of prior approval are difficult and time-consuming.
Physician and patient wait times increase while the provider loses out on precious time. After the pandemic, healthcare workers have either switched jobs or are under huge stress. Reallocation of the resources to look at important jobs like patient care still looks far-fetched for many hospitals.

Outpatient Procedures That Need Prior Authorization
- Cosmetic or reconstructive surgery and other procedures
- Pulmonary rehabilitation and outpatient cardiac treatment
- Home healthcare services: agency visits, sleep studies, hospice care excluding home visits that are billed as an E&M service.
- Ambulatory surgery center based infusion services as well as associated medications
- Genetic testing and elective transportation services
- Durable Medical Equipment services
- Stem cell and organ transplant procedures
- Mental & behavioral health treatment
- Radiology services
- GI medication
- Pharmacy
- Injectable medication
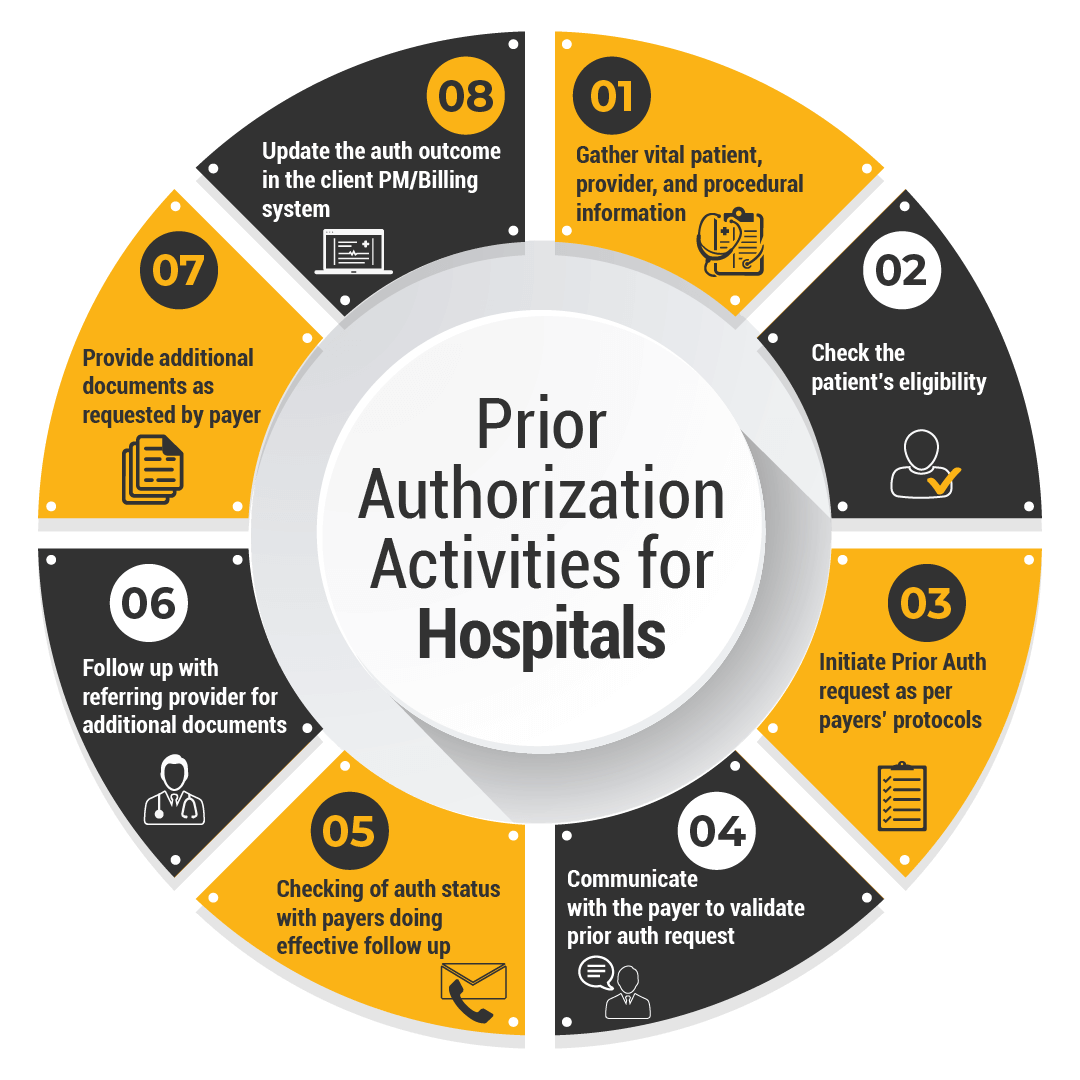 It is quite evident that as a hospital managing your patients and prioritizing a better practice management effort is a challenge. Moreover, the lack of expert resources is a huge setback for healthcare providers at present.
It is quite evident that as a hospital managing your patients and prioritizing a better practice management effort is a challenge. Moreover, the lack of expert resources is a huge setback for healthcare providers at present.
Rising operational costs, pending backlogs, and denials are posing a serious threat to many. The need of the hour is to find someone consistent and trustworthy, a partner that can deliver the right support in your hospital prior authorization process.
Partner with us in these difficult times
Worry no more when we are by your side! We are a complete healthcare RCM service destination; understand what it takes to transform your cash flow. Our team of experts understands the present-day industry challenges, drivers and restraints, and extends superior support in outpatient hospital prior authorization. We help you gain the right visibility in your front-end efforts, and help you save time and money. Our team will help in eliminating
Absence of visibility in the Authorization Process
Higher
Employee Workload
Lack of
Patient Focus
With an extensive understanding of individual payer requirements, our team completes all the functions by:
![]() Verifying eligibility
Verifying eligibility
![]() Initiating authorization
Initiating authorization
![]() Following up on the request
Following up on the request
![]() Obtaining and acknowledging authorization
Obtaining and acknowledging authorization
![]() Scheduling the procedure
Scheduling the procedure
We ensure
![]() 100% PA submission on the same day itself
100% PA submission on the same day itself
![]() 99% accuracy
99% accuracy
![]() Assisting you schedule procedures within 48 hours
Assisting you schedule procedures within 48 hours
![]() Saving your practice time and money
Saving your practice time and money
![]() Redeploying your resources to core functions of patient care
Redeploying your resources to core functions of patient care
![]() Reducing cost by 80%… guaranteed!
Reducing cost by 80%… guaranteed!
The best part, all our services are placed at $7 per hour with a full-time resource working only for you. Speak to a Sunknowledge expert right now and transform your flow of revenue without worrying about running short of resources.
