Credentialing is the process of obtaining, verifying, and evaluating the qualifications of a provider and determining whether an applicant is qualified is qualified to be a participating provider with the organization.
Sunknowledge is happy to aid provider groups as well as clients with a complete range of credentialing services through a time-tested technique that ensures that organizational providers are compliant with state and regulatory bodies before directing membership to these facilities.
Proper credentialing requires a watchful eye on total and stringent compliance with applicable standards. It also requires that applicants are evaluated in the right manner and their competencies are measured accurately. For this, a number of resources are consulted such as the social, academic, and professional history of the applicant, peer and expert reviews, end-user reviews on the quality of the applicant’s services, and more.
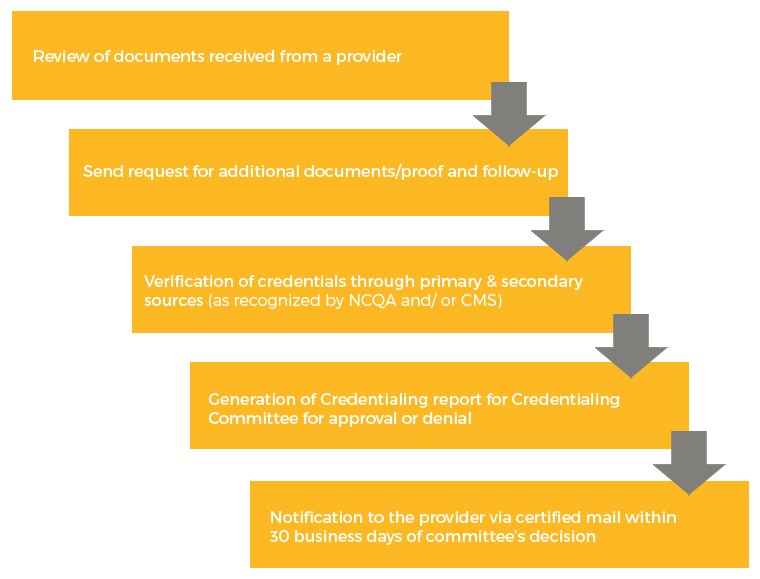
At Sunknowledge, we are fully equipped to take care of all these requirements quickly and efficiently. We approach the subject in an organized and systematic manner. The key steps in our credentialing process are as follows:
Highlights
- Full range of credentialing services
- Re-credentialing after every 3 years
- Regular updates of provider data in credentialing and claims systems
- Generation of all pertinent reports like
- HSD Report
- Physician and Facility Reports
- Weekly ADD/TERM report
- Delegated credentialing report
- Group/taxonomy etc. specific ad-hoc reports
At Sunknowledge, we work with a full team of credentialing veterans who strictly abide by the standards and guidelines set within Medicare Managed Care Manual and National Committee for Quality Assurance (NCQA). So, why look anywhere else?
