Like many practices, Infusion Prior Authorization Services play a vital role. As a responsible infusion practice owner, your primary objective is to ensure the best patient care which ensures the right prior authorization operation, while safeguarding your cash flow. According to a survey conducted by the American Medical Association (AMA) in 2021, 62% of physicians expressed challenges in discerning whether prior authorization is required for medical services. Extensive process: Most healthcare find prior authorization services for infusion as a time-consuming affair. Pre-auth requires detailed documentation and obtaining approval may take a few weeks or a month. It may hinder the care. Administrative burden: The amount of paperwork and documentation required by the PA process often poses an extra burden for infusion specialists. The whole process takes up a significant amount of time from delivering patient care. Ambiguous process: The complex criteria of prior authorization for infusion practices can be ambiguous for a lot of infusion practices. The complex nature of pre-auth often leads to errors, misunderstanding, and requirements for additional documents, further delaying patient care. No standard requirements: Different insurance companies have different PA requirements for the same medical procedure or medication. Denials and appeals: The reason behind an authorization denial may not always be clear, making it difficult for providers to address the specific issue. Patient frustration: Patients get frustrated often for not receiving timely treatments or medications. Understanding prior authorization and dealing with denials cause stress for patients. Unfortunately, most infusion practices don’t have sufficient budget to build a team of experienced and skilled prior auth experts from scratch. You cannot afford to ignore adhering to payers’ guidelines linked to your facility, including service delivery locations, treatment expenses, medication preferences, and coverage status for intricate and crucial procedures. With all these details to register, you need an expert to administrator the prior authorization process. And also, as infusion practices deal with a wide area of clinical care for their patients and often struggle to manage a critical administrative; it’s best that you have an expert by your side. Additionally, specific emergencies may arise, necessitating pre-approval exceptions in certain cases. Are you also in the same pool of frustration? So, what’s the best solution? Outsource Infusion Prior Authorization Services to Sunknowledge. We, at Sunknowledge, bring our domain-leading experience and skills-set to the table to streamline the end-to-end Prior Authorization Services for Infusion. With more than 18 + years of extensive industry experience, we have been providing top-notch Infusion Prior Authorization Services to reputed practices across 50 states. We always leverage advanced technologies to mitigate human errors, cut down operational costs and TAT giving a strong boost to your practice’s revenue. Our pricing model- $7/FTE, is designed to meet the needs of businesses of all sizes. We offer flexible options for part-time or full-time support, allowing you to choose the level of assistance that best suits your requirements. Additionally, our team of experienced professionals is dedicated to delivering high-quality results and exceeding client expectations. What sets us apart from other participants in the Pre-Auth market is our exceptional ability to secure prior authorization for insurance reimbursement, particularly for quasi-medical products like Botox, commonly utilized for cosmetic purposes. Many prior authorization companies often consider this task nearly impossible, but we excel in achieving it. So, what are you waiting for? Enjoy healthy cash flow along with ensuring patient-satisfaction by outsourcing infusion prior authorization services to us. If you want to know more about our RCM solutions, schedule a no-obligatory call with us and we would love to assist you.Key challenges with Prior Authorization Services for Infusion:

Sunknowledge: One of the best infusion prior authorization companies!
Our infusion prior authorization services involve seven critical steps:
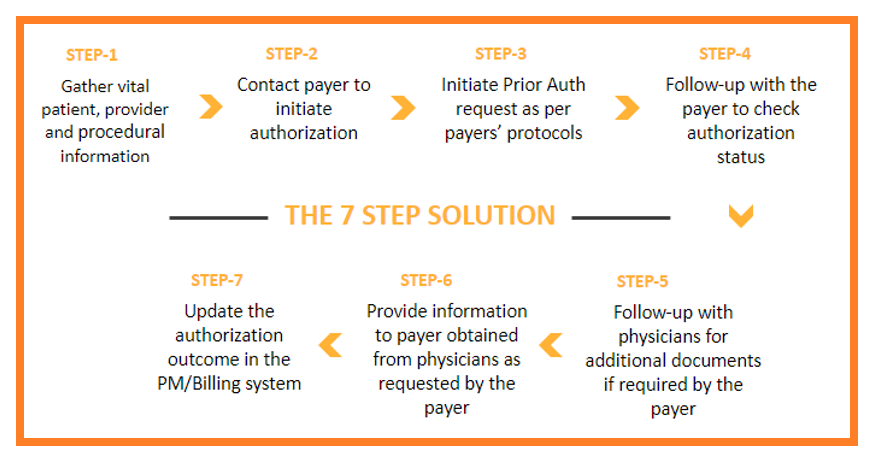
Outsource Infusion Prior Authorization Services and Enjoy the following Benefits:
Call us at (646) 661-7853
Carnegie Hall Tower, 59th Floor, New York, NY 10019
